October 02, 2014
In the past few months, it has become evident that Illinois vastly underestimated the number of newly eligible recipients who would sign up for Medicaid under the Affordable Care Act. However, the fiscal implications of the unexpectedly strong enrollment remain unclear.
Governor Pat Quinn said on September 30, 2014 that 468,000 newly eligible individuals had enrolled in Illinois’ Medicaid program. The Governor made the announcement at an event marking the one-year anniversary on October 1 of the initial sign-up period for enrollment in the expanded Medicaid program and the new insurance exchanges mandated by the Affordable Care Act (ACA). Total Medicaid enrollment for comprehensive benefits stood at 2.8 million at the end of June 2013.
The enrollment by newly eligible recipients is nearly triple initial projections by the Illinois Department of Healthcare and Family Services (HFS), the State’s main Medicaid agency. As discussed here, HFS initially projected that 161,000 newly eligible individuals would sign up by the end of the 2014 fiscal year on June 30, 2014 and 342,000 would enroll by the end of calendar year 2017.
The initial forecast was part of the Governor’s recommended FY2014 budget released in March 2013, nine months before the Medicaid expansion took effect on January 1, 2014. In March 2014, in connection with the Governor’s proposed FY2015 budget, State officials increased the enrollment estimate for newly eligible recipients to 350,000 by the end of FY2014 and 385,000 by the end of FY2015.
Medicaid is a joint federal-state program that pays for healthcare for certain categories of low-income citizens, including children, pregnant women, parents, the disabled and the elderly. The ACA gave states the option of providing Medicaid to the major population that generally had not been covered: non-elderly, non-disabled adults without dependent children. For states that chose to participate, the ACA extended Medicaid coverage to such adults with incomes up to 138% of the federal poverty level (meaning that a single person can have income up to $16,105 in 2014).
The General Assembly approved Illinois’ participation in the expansion at the end of the spring 2013 legislative session.
Newly eligible recipients were not the only individuals expected to sign up for Medicaid as a result of the ACA. Illinois and other states also expected previously eligible individuals who had not signed up for Medicaid to enroll in the program because of publicity surrounding the ACA and policies that steer individuals to Medicaid if they are not eligible to obtain insurance coverage through the new insurance exchanges.
HFS initially projected that about 80,500 previously eligible individuals would enroll in the program by the end of FY2014 because of the ACA. That number was expected to grow to 167,000 by the end of 2017, bringing total ACA-related enrollment to 509,000. The estimate for FY2014 was reduced slightly to 80,000 in connection with the FY2015 budget.
The agency has not issued a new estimate of enrollment by previously eligible recipients, and it appears that this category of participation might have become difficult to track. HFS had planned to base its estimate on the growth in enrollment that exceeded trend rates. However, the State is proceeding with the Medicaid Redetermination Project, an effort to remove ineligible recipients from the program’s rolls by cross-checking electronic data on recipients’ income, employment and address. It appears that the results of that project, combined with an improving economy, might offset any enrollment increases due to previously eligible ACA participants.
The following table compares actual enrollment of newly eligible recipients as of September 2014 with various State projections. A new estimate has not been issued for 2017. It should be noted that Medicaid enrollment figures as of a specific date change over time because recipients are potentially eligible for retroactive coverage for incurred health care costs dating back to 90 days prior to the date of application.
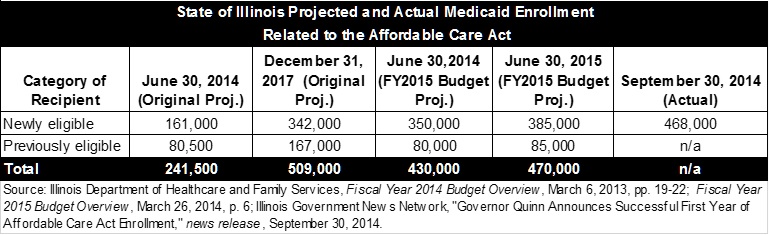
Whether ACA participants are newly eligible or previously eligible makes a big difference for the State budget. State Medicaid expenditures are generally reimbursed by the federal government at a rate known as the Federal Medical Assistance Percentage (FMAP), which varies by state depending on per capita income. The federal matching rate for Illinois increased to 50.76% for the federal fiscal year that began on October 1, 2014 from 50.0% for the previous fiscal year.
While State costs for previously eligible Medicaid recipients are reimbursed at the regular matching rate, the federal government is scheduled to pay 100% of the cost for the newly eligible ACA population for the first three years of the program, through calendar year 2016. The reimbursement rate declines to 95% in 2017, 94% in 2018, 93% in 2019 and 90% thereafter.
HFS estimated total ACA-related costs (paid by both the federal government and the State) in FY2014 at $604.1 million. The figure included $491.7 million for newly eligible recipients and $112.4 million for previously eligible recipients.
Total ACA-related costs were projected to more than triple to $2.15 billion in FY2015. The total includes $1.76 billion for newly eligible recipients and $392.9 million for previously eligible individuals.
Illinois is not the only state experiencing unexpectedly strong ACA enrollment. California reportedly had an increase in Medicaid enrollment of 2.2 million since January 2014, bringing its total number of recipients to 11 million. It is not clear how many of California’s new enrollees are newly eligible and how many were previously eligible.
Federal statistics on Medicaid enrollment do not separate newly eligible individuals from other new enrollees. According to the Kaiser Family Foundation, many state computer systems are unable to track enrollment in this group separately and provide data immediately.
Across the U.S., enrollment as of July 31, 2014 was 67.2 million, or 8 million higher than average monthly enrollment prior to October 2013, according to the latest preliminary data from the federal Centers for Medicare and Medicaid Services. The growth rate was 20.3% in the 26 states and the District of Columbia where the ACA expansion had been implemented as of July 2014, compared with 4.8% in states that had not expanded the Medicaid program. Connecticut and Maine were not included because they did not submit data for the baseline period.
